Diabetic retinopathy treatment may be needed the longer a person lives with diabetes. This explains the reason why each year an increasing number of people experience loss of eye sight and other issues linked with diabetes.

Diabetic Retinopathy Treatment Options
by CRfan
The risk for diabetic retinopathy increases the longer a person has lived with diabetes. Treatment revolves around laser treatment and injections.
Background and Demographics
Type II diabetes represents 90% of all patients with diabetes. Since Type II diabetes rarely has any symptoms associated with it, a great deal of cases remain undiagnosed for long time periods. Twenty percent of them will need diabetic retinopathy treatment after they get diagnosed with diabetes and more than 60% will experience retinopathy fifteen years after a diagnosis.
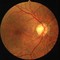
The secret to controlling eye problems with diabetes is by having regular eye exams. The eye is the only body part in which small to medium size blood vessels and those which have been impacted can be viewed without an operation. A dilated eye exam allows an eye doctor to understand what is going on in the eye as well as provide them an image of the patient’s overall wellness. They may assist in the management of diabetes in collaboration with a general health care provider along with other specialists in the medical field like neurologists. Diabetic care calls for a team of qualified physicians.
Diabetes makes the eyes lose their tight seals and then blood will start to leak from them. Fresh blood vessels may form as an effort to feed tissues that need nourishment. The thing is these newly created blood vessels do more damage since they have a tendency to leak extra VEGF or Vascular Endothelial Growth Factor.
Macular Edema is the main reason diabetics have trouble with their vision. It is also known as Clinically Significant Macula Edema (CSME). DME results in fluid accumulation beneath the macula which is section of the retina that is responsible for our sharpest vision. The fluid buildup makes the retina swell, resulting in loss of eyesight.
Types of Laser Treatment in Diabetic Retinopathy
Each diabetic retinopathy treatment with lasers focuses on helping the patient keep their remaining eyesight. The aim is to make the damage to the retina stabilize and prevent further eyesight loss.
- Laser Photocoagulation: This is the usual retinopathy treatment. Photocoagulation diabetic retinopathy treatment applies a laser to destroy the damaged sections of the retina so the most important sections like the macula get the blood it needs without leaking. However, that is not accomplished without a side-effect. Destroying parts of the retina can result in loss of peripheral vision.
- Panretinal or Scatter Photocoagulation: This type of retinopathy laser treatment can produce as many as 2000 burns in the retina’s exterior. Patients with proliferative diabetic retinopathy often undergo this type of laser treatment that treats neovascularization sections indirectly.
- Focal or Focus laser treatment: This type of treatment involves perfectly aimed shots designed to destroy blood vessels in a set pattern. Grid laser therapy is typically reserved for those with DME.
Fluorescein angiography helps pinpoint the blood vessel leakage in areas that need treatment.
Panretinal Photocoagulation (PRP)
Vitrectomy
Every now and then, bleeding coming from the diabetic ey will leak into the vitreous humor and it still may not recede once the retina has received treatment. You may need to have the vitreous humor taken out. In a few situations, the blood is very widespread and it prevents the doctor from viewing the retina and hinders their ability to operate. The doctor may proceed to take out the vitreous and may opt to use laser treatment as they stay in the eye or at a follow-up appointment through a dilated pupil. When the vitreous is filled with blood, it can result in bands of fibrotic scar tissues being created which constrict and pull on the retina.
Non-Laser Treatments
Steroid injections can take the place of retinopathy laser treatments. These are applied in two ways. One is by an insert that slowly discharges the steroid in the retina and the other method is by a solution injected into the vitreous cavity.
Triamcinolone acetonide (Kenalog) is injected more frequently. This works by bringing down the swelling and works to cut DME by stopping fresh absorbent blood vessels from being created. Retisert Bausch & Lomb)and Ozurdex (Allergan) are two brands of intravitreal inserts to treat DME.
These injections have side-effects associated with them as with any other types of steroids. A few side-effects are an increased risk of steroid-produced glaucoma, cataracts, and endophthalmitis.
More Diabetic Retinopathy Treatments
Certain Anti-VEGF injections are often employed by some doctors to treat proliferate retinopathy. These have been approved to treat wet macular degeneration. Doctors find these successful in treating eye problems linked with diabetes because the diabetics’ blood vessels are prone to leakage, much like the blood vessels in wet macular degeneration. Avastin, Macugen and Lucentis are treatments used for injection into the vitreous one time per month or every other month for macular degeneration However, diabetic retinopathy is not as predictable and the symptoms can get better once treatment has started. Due to this, the injections may not have to be used as often and they have been proven to be successful. Bayer Company formulated VEGF Trap-Eye (Eylea) in collaboration with Regeneron which has been showing high rates of success for diabetes and other conditions. Japan and Europe started clinical trials in 2011 and the trials in the United States will be conducted at a future time.
You might also like
Thyroid Cancer - What To Expect When You've Been DiagnosedEverything you need to know about thyroid cancer, from diagnosis to types of ...
Anosmia - Can it be reversed ?Anosmia- loss of the sense of smell is one of the first signs of Parkinson's ...


 How The FDA Approves New Medicineson 08/16/2013
How The FDA Approves New Medicineson 08/16/2013
 10 Tax Mistakes Business Owners Makeon 08/05/2013
10 Tax Mistakes Business Owners Makeon 08/05/2013
 Accessories For Traveling With Jeweleryon 02/12/2013
Accessories For Traveling With Jeweleryon 02/12/2013
 Stages of the Sleep Cycleon 09/23/2012
Stages of the Sleep Cycleon 09/23/2012

Comments