We are quite literally bacterial worlds. Though a lot of what we shelter in the form of flora is benign some must also be beneficial.
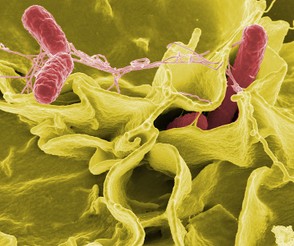
True, we are all painfully aware of the publicized warnings about salmonella and e.coli. If we are paying the least bit of attention, we know where in our food supply the contaminants are, how they got there, and what authorities are recommending we should be doing about it.
What many of us don’t realize is that almost every one of us gives refuge to a colonies of these very same bacteria at all times.
E. coli has a number of “versions;” some of which are benign and some of which are dangerous. In fact, most of the strains that we play host to are harmless. Recently, however, researchers in Norway discovered that a virus can actually alter the good e. coli, and convert it to a bad variety.
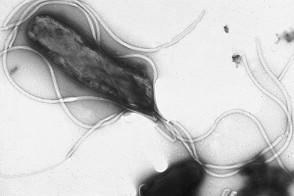
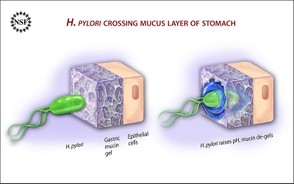
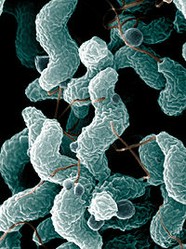
Before the advent of antibiotics, almost every American sheltered Helicobacter pylori. This is a particularly troubling bacterium as it has been linked to ulcers and stomach cancer in adults and children. Since the advent of antibiotics that number, as a percentage of the population, has dropped drastically; well below 10% of the population.
In premature infants, h. pylori has been implicated in the gastritis, peptic ulcers, and, worst of all, necrotizing enterocolitis. Necrotizing means tissue death and enterocolitis is an inflammation in the gut. This last, typically only seen in preemies, is deadly and very hard to halt once an infection takes hold. It is a fast moving bug, often becoming a life threatening condition literally over-night. An h. pylori infection unless treated early and aggressively results in death. The problem for medicine is spotting it in time and treating it promptly. To that end knowing more about an infant’s microbial load and make-up is vital.
If we all play host to these and other bacteria, the question must be “what keeps them from making us sick?” This article will not only attempt to answer that question, but present you with information that may surprise you.

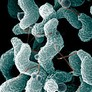
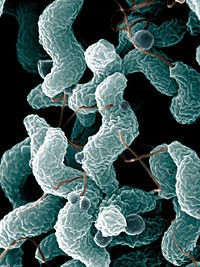 However, this view is undergoing a radical change. For most of us, playing unintentional host to ten times our own cell count in bacteria, these “guests” pose no risk. Indeed the bacteria we play home to seem beneficial in some situations or benign in others. As of this writing scientists have identified over ten thousand species of bacteria living upon or within the average human being. With over one hundred different types living behind the ear, a thousand different varieties in the mouth and hundreds of other genus living upon our hands, our bodies are quite literally home to a galaxy of living microorganisms.
However, this view is undergoing a radical change. For most of us, playing unintentional host to ten times our own cell count in bacteria, these “guests” pose no risk. Indeed the bacteria we play home to seem beneficial in some situations or benign in others. As of this writing scientists have identified over ten thousand species of bacteria living upon or within the average human being. With over one hundred different types living behind the ear, a thousand different varieties in the mouth and hundreds of other genus living upon our hands, our bodies are quite literally home to a galaxy of living microorganisms.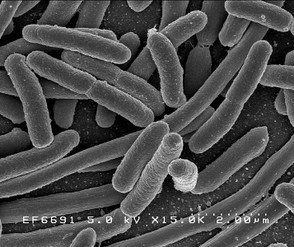

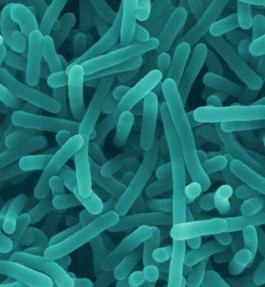 Bacteria have also been implicated in stubborn weight gain. Cursory studies have found that people who just cannot seem to keep the weight off have a overabundance of bacteria types called firmicutes. Laboratory mice which have been bred with no bacteria at all then “infected’ with firmicute type bacteria, experience sudden weight gain. A control group of mice, who lacked these types of microbes and were fed exactly the same diet, maintained normal weight. Are firmicutes somehow able to make digestion and nutrient extraction more efficient?
Bacteria have also been implicated in stubborn weight gain. Cursory studies have found that people who just cannot seem to keep the weight off have a overabundance of bacteria types called firmicutes. Laboratory mice which have been bred with no bacteria at all then “infected’ with firmicute type bacteria, experience sudden weight gain. A control group of mice, who lacked these types of microbes and were fed exactly the same diet, maintained normal weight. Are firmicutes somehow able to make digestion and nutrient extraction more efficient?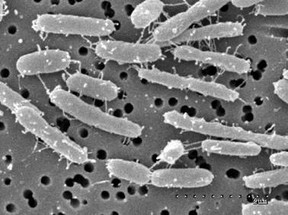 On the opposite end of the diet scale scientists have also discovered that people who have an overabundance of bacteroidetes seemed to be able to eat any amount and or type of food with weight gain impunity. This has also been borne out with rodent studies similar to the study mentioned above.
On the opposite end of the diet scale scientists have also discovered that people who have an overabundance of bacteroidetes seemed to be able to eat any amount and or type of food with weight gain impunity. This has also been borne out with rodent studies similar to the study mentioned above.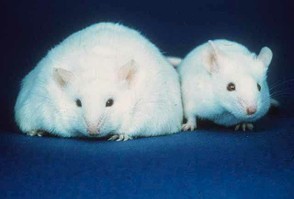


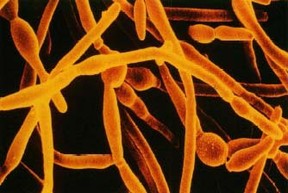 Antibiotic use in children has been linked to rashes, stomach ache, and diarrhea. Continual use has also been linked to Candida overgrowth which, in turn, is linked to life-long problems with headache, acne, eczema, PMS, athlete's foot, cancer, allergies, depression, chronic fatigue, vision problems, sinus problems, ear problems, yeast infections, mood swings, irritable bowel syndrome, constipation, poor memory, chronic pain, and acid reflux disease. The root cause of this “overgrowth” seems to be the wiping out of bacteria that prevent Candida from taking over in the first place.
Antibiotic use in children has been linked to rashes, stomach ache, and diarrhea. Continual use has also been linked to Candida overgrowth which, in turn, is linked to life-long problems with headache, acne, eczema, PMS, athlete's foot, cancer, allergies, depression, chronic fatigue, vision problems, sinus problems, ear problems, yeast infections, mood swings, irritable bowel syndrome, constipation, poor memory, chronic pain, and acid reflux disease. The root cause of this “overgrowth” seems to be the wiping out of bacteria that prevent Candida from taking over in the first place.




 Crêpes and Crêpe Disheson 09/14/2016
Crêpes and Crêpe Disheson 09/14/2016
 About Me - Liam Beanon 11/28/2014
About Me - Liam Beanon 11/28/2014
 About Ebolaon 11/08/2014
About Ebolaon 11/08/2014



Comments
Thanks for the keen insight Elias. I agree completely!
I agree that this is a subject that requires further scientific research and also deserves more awareness on behalf of the people. For all the good that modern medicine has offered there are critical issues such as those you mention here, that should not be overlooked. The transformation of old microorganism into new, treatment resistant forms could be really worrying especially in relation to the fact that modern antibiotics have largely altered/weakened even destroyed our immune system.
Thanks Frugalrvers. This has been in the news so much I thought it time to try to tackle the subject. I'm no M.D., but as an amateur scientist (in other words an unpaid information junkie) I thought it was time. I was inspired by news reports, an article in Smithsonian, an announcement (very recent) by Consumer Union regarding salmonella, and all the recent warnings by the CDC.
Though there is no hard information on precisely what bacteria are truly "bad," the correlative studies are intriguing. The Finnish study in particular is very interesting.
Maybe that's why I'm so disgustingly healthy with no allergies. In my youth I went without shoes, played in dirt, drank from the garden hose, and rarely washed my hands. Of course, once I hit my teens all that changed, but perhaps by then all those bugs gave my immune system the workout boost it needed.
Such a great article!
A decade ago, I was an antibiotic junkie...until my body started falling apart.
Fast forward to today and my holistic MD and I just never catch anything anymore. I keep my immune system strong with dandelion root, maitake and garlic and just never get sick. I used to catch anything and everything! Absolutely, if I was gravely ill and losing the battle, I would take an antibiotic - but only as a last resort.